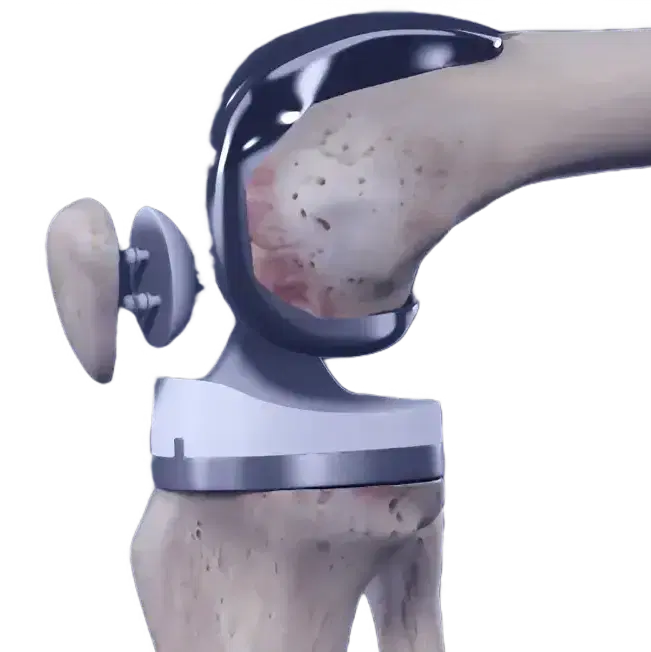
What is
ACL Reconstruction
ACL (anterior cruciate ligament) surgery is a procedure used to repair or reconstruct the ACL, a ligament in the knee that helps stabilize the joint
ACL surgery is common for sports-related complete or partial ACL tears. It uses autograft/allograft to replace the damaged ligament. Recovery takes several months for full knee healing and function.
What is your Anterior Cruciate Ligament (ACL)
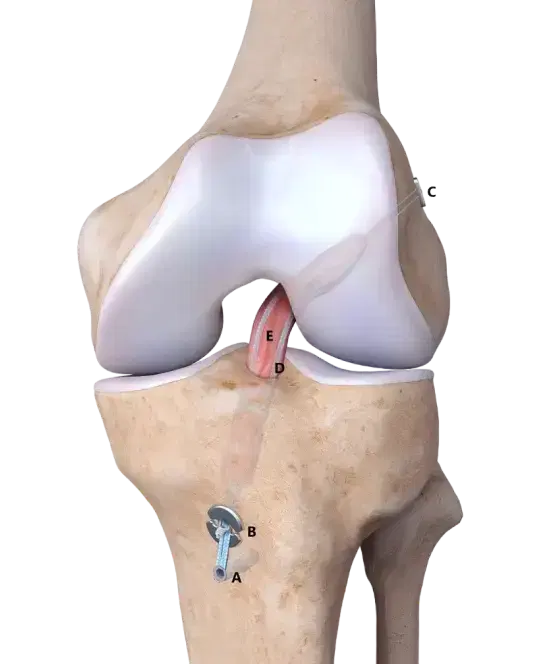
The anterior cruciate ligament is one of the major stabilizing ligaments in the knee. It is a strong rope- like structure located in the centre of the knee running from the femur to the tibia.
When this ligament tears, unfortunately, it doesn’t heal and often leads to the feeling of instability in the knee.
The ACL is the major stabilizing ligament in the knee. It prevents the tibia (shin bone) moving abnormally on the femur (thigh bone). When this abnormal movement occurs, it is referred to as instability and the patient is aware of this abnormal movement.
An ACL reconstruction is a commonly performed surgical procedure and with recent advances in arthroscopic surgery can now be performed with minimal incisions and low complication rates.
Often, other structures such as the meniscus, the articular cartilage (lining the joint) or other ligaments can also be damaged at the same time as a cruciate injury and these may need to be addressed at the time of surgery.
1
Most injuries are sports-related involving a twisting injury to the knee.
2
It can occur with a sudden change of direction, a direct blow, e.g., a tackle, landing awkwardly.
3
Often there is a popping sound when the ligament ruptures.
4
Swelling usually occurs within hours.
5
There is often the feeling of the knee popping out of joint.
6
It is rare to be able to continue playing sports with the initial injury
Once the initial injury settles down, the main symptom is instability or giving way of the knee. This usually occurs with running activities but can occur with simple walking or other activities of daily living
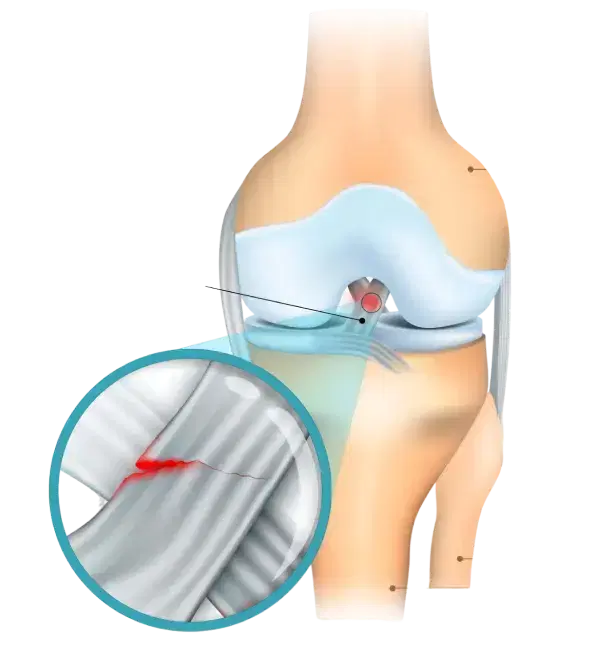
ACL Injury Diagnosis
The diagnosis can often be made on history alone.
Examination reveals the instability of the knee if adequately relaxed or not too painful.
An MRI (Magnetic Resonance Imaging) can be helpful if there is a doubt, or to look for damage to other structures within the knee.
At times the final diagnosis can only be made under an anesthetic or with an arthroscopy.
What Are The Treatment Options?
Rest
Elevation
Ice
Bandage
Long term
Not everyone needs surgery. Some people can compensate for the injured ligament with strengthening exercises or a brace.
It is strongly advised to give up sports involving twisting activities if you have an ACL injury.
Episodes of instability can cause further damage to important structures within the knee that may result in early arthritis
What Are The Indications for ACL Surgery?

Young patients wishing to maintain an active lifestyle.

Sports involving twisting activities, e.g., soccer, netball, football Giving way with activities of daily living.

People with dangerous occupations, e.g., policemen, firemen, roofers, scaffolders.

Pre-surgery physiotherapy helps improve motion and muscle strength.
How is an ACL
Reconstruction Performed?
Surgical techniques have improved significantly over the last decade, complications are reduced and recovery much quicker than in the past.
The surgery is performed arthroscopically
What do the post-operative steps include?
Surgery is performed as a day procedure or an overnight stay.
You will have pain medication by tablet or in a drip (Intravenous).
Any drain will be removed from the knee.
A splint is sometimes used for comfort.
You will be seen by a physiotherapist who will teach you to use crutches and show you some simple exercises to do at home.
Leave any waterproof dressings on your knee until your post-op review.
You can put all your weight on your leg.
Avoid any anti-inflammatory or aspirin for 10 days.
Put ice on the knee for 20 minutes at a time, as frequently as possible.
Post-op review will usually be after about 7-10 days.

Rehabilitation for ACL
Reconstruction
Physiotherapy is crucial for treatment and starts early.
Pre-operative physio helps prepare the knee. Early goals are range of motion, reduced swelling, and full weight-bearing.
Supervised rehab includes biking, swimming, proprioceptive exercises, and muscle strengthening. Cycling at 2 months, jogging at 3 months, and sports at 6 months (subject to factors). Recovery time varies; rehab success depends on associated knee injuries.
A detailed rehab protocol is provided for patients and physiotherapists, adaptable to individual needs.
Stage 1 Acute (0 – 2 Weeks)
Goals
Wound healing
Reduce swelling
Regain full extension
Full weight-bearing
Wean off crutches
Promote muscle control


Treatment Guidelines
Pain and swelling reduction with ice, intermittent pressure pump, soft tissue massage and exercise.
Patella mobilization.
Active range of motion knee exercises, calf and hamstring stretching, contraction (non- weight-bearing progressing to standing), muscle control and full weight-bearing. Aim for a full extension by 2 weeks. Full flexion will take longer and generally will come with gradual stretching. Care needs to be taken with hamstring co-contraction as this may result in hamstring strains if too vigorous. Light hamstring loading continues into the next stage with the progression of general rehabilitation. Resisted hamstring loading should be avoided for approximately 6 weeks.
Gait retraining encouraging extension at heel strike
Stage 2 Quadriceps Control (2-6 Weeks)
Goals
Full active range of motion.
Normal gait with a reasonable weight tolerance.
Minimal pain and effusion.
Develop muscular control for controlled pain-free single leg lunge.
Avoid hamstring strain.
Develop early proprioceptive awareness.


Treatment Guidelines
Use active, passive and hands-on techniques to promote a full range of motion.
Progress to closed chain exercises (quarter squats and single-leg lunge) as pain allows. The emphasis is on pain-free loading, VMO and gluteal activation.
Introduce gym-based exercise equipment including leg press and stationary cycle.
Water-based exercises can begin once the wound has healed, including treading water, gentle swimming avoiding breaststroke.
Begin proprioceptive exercises including single standing leg balance on the ground and mini-tramp. This can progress by introducing body movement whilst standing on one leg.
Bilateral and single calf raises and stretching.
Avoid isolated loading of the hamstrings due to ease of tear. Hamstrings will be progressively loaded through the closed chain and gym-based activity.
Stage 3 Hamstring/Quadriceps Strengthening (6-12 Weeks)
Goals
Begin specific hamstring loading.
Increase total leg strength.
Promote good quadriceps control in lunge and hopping activity in preparation for running.


Treatment Guidelines
Focal hamstring loading begins and is progressed steadily throughout the next stages of rehabilitation:
- 1. Active prone knee flexion, gradually adding lightweight and increasing weights.
- 2. Bilateral bridging off a chair, then progress to single leg bridge with weight held across abdomen.
- 3. Single straight leg deadlift, increase difficulty with dumbbells.
- 4. Avoid pushing hamstrings into pain, progress carefully, reduce exercises if strain or tightness occurs.
Gym based activity including leg presses, light squats and stationary bike which can be progressively increased in intensity as pain and control allow. It is important to monitor any effusions following exercise and if it is increasing then exercise should be toned down.
Once single leg lunge control is comparable to the other side, hopping can be introduced. Hops can be made more difficult by including variations such as forward/back, side to side off a step and in a quadrant.
Running may begin towards the latter part of this stage.
Increased proprioceptive manoeuvres with standing leg balance and progressive hopping based activity.
Expand the calf routine to include eccentric loading.
Prior to running, certain criteria must be met:
- 1. No anterior knee pain.
- 2. A pain-free lunge and hop that is comparable to the other side.
- 3. The knee must have no effusion.
- 4. Before jogging start having brisk walks, ideally on a treadmill to monitor landing.
- 5. Action and any effusion- this should be done for several weeks before jogging properly.
Stage 4 Sport Specific (3-6 Months)
Goals
Improve leg strength
Develop running endurance speed, change of direction
Advanced proprioception
Prepare for return to sport and recreational lifestyle


Treatment Guidelines
Controlled sport specific activities should be included in the progression of running and gym loads. Increasing effusion post running that isn’t easily managed with ice should result in a reduction in running loads
Advanced proprioception to include controlled hopping and turning and balance correction
Monitor potential problems associated with increasing loads
No open chain resisted leg extension exercises unless authorized by your surgeon
Stage 5-Return to Sport (6 Months Plus)
Goals
A safe return to sporting activities


Treatment Guidelines
Full training for 1 month prior to active return to competitive sport.
Preparation for body contact sports. Begin with low-intensity one on one contests and progress by increasing intensity and complexity in preparation for drills that one might be expected to do at training.
To improve running endurance leading up to a normal training session.
Full range, no effusion, good quadriceps control for lunge, hopping and hop and turn type activity. Circumference measures of thigh and calf to within 1 cm of the other side.
Risks & Complications of
ACL Reconstruction
Complications are not common but can occur. Prior to making the decision to have this operation, it is important you understand these so you can make an informed decision on the advantages and disadvantages of surgery.
These can be medical (Anesthetic) complications and surgical complications.
A classic history with location of pain and exacerbating factors
Have restricted mobility that is interfering with their lifestyle
1
Infection (Approx. 1 in 200): Treated with antibiotics or, in rare cases, further surgery to clean the infection
2
Deep vein thrombosis: Blood clots in leg veins may require blood-thinning medication or pose risk of pulmonary embolism (breathing difficulties or death).
3
Excessive swelling & bruising: Resulting from soft tissue bleeding, usually resolves with time.
4
Joint stiffness: Scar tissue can cause limited movement, but advances in surgery and rehab minimize this.
5
Graft failure (Approx. 5%): Graft can fail, but it can be revised using tendons from the other leg.
6
Damage to nerves or vessels: Small nerves under the skin can cause numbness, rarely affecting important nerves.
7
Hardware problems: Devices used to fix graft may cause irritation and may need removal later.
8
Donor site problems: Hamstrings or patella tendon used as graft sources may cause temporary pain or swelling.
9
Residual pain: May occur, especially if other knee structures are damaged.
10
Summary: ACL reconstruction is common and successful, recommended for active individuals, especially those in sports involving running and twisting.

Do you need a
Knee replacement?
Dr Seeto in affiliation with Medibank Private and East Sydney Private hospital, offers a program for eligible Medibank Private Members, to eliminate medical out of pocket costs for your Knee Replacement.
The program includes a pre-surgery preparation program, spending the minimal time necessary in hospital, as well as home rehabilitation if necessary.
Book a consultation
today
9:00 am - 4:30 pm